“Sleep is the chief nourisher in life’s great feast”
Macbeth, Shakespeare
At the start of every year there is always a lot of talk about refraining from certain activities like drinking alcohol, advice about eating a particular way, or recommendations to do certain types/amount of exercise. Trends in these lifestyle choices may come and go, but there is one behaviour that remains constant to achieve optimal health. Sleep.
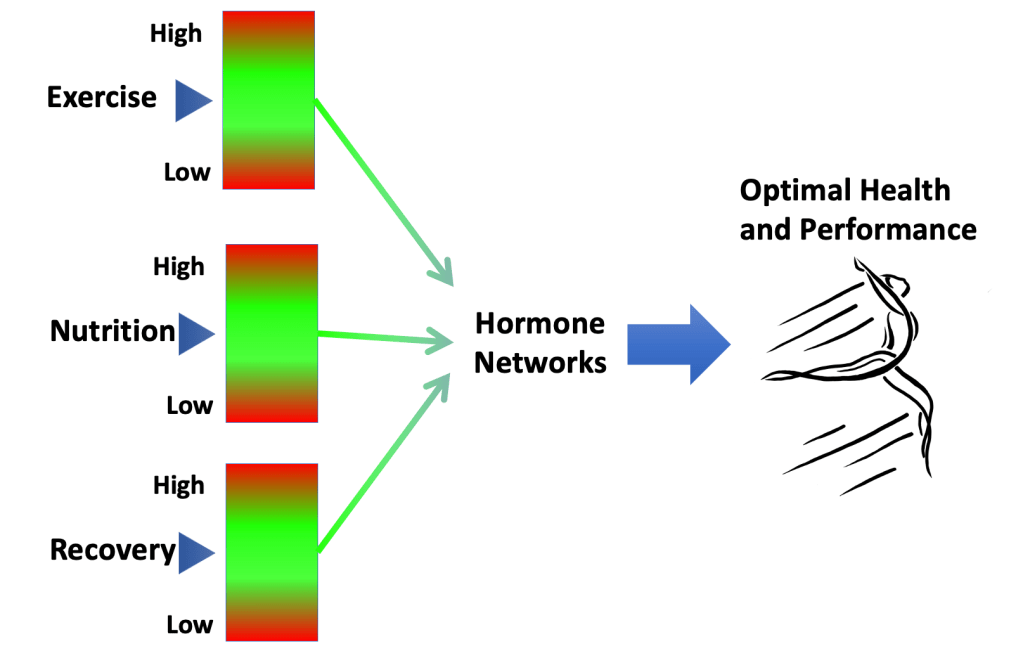
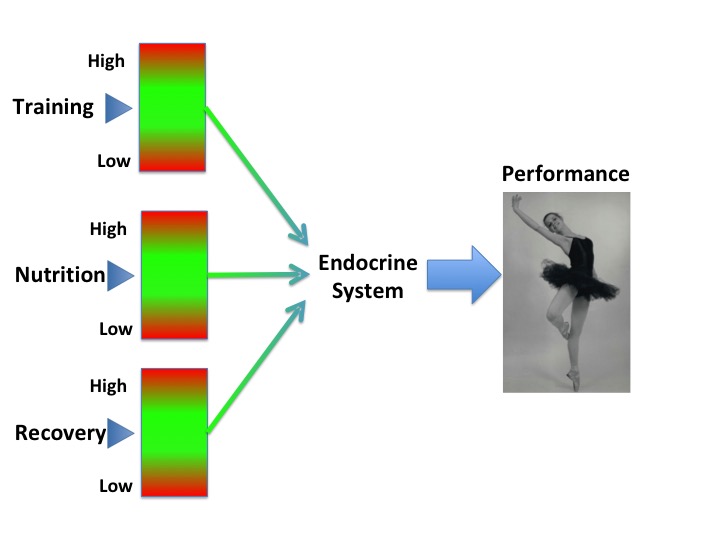
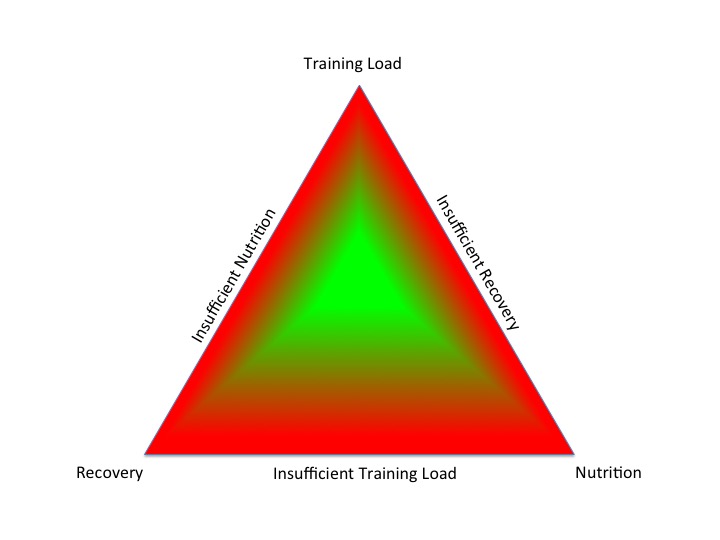
In my book “Hormones, Health and Human Potential: A guide to understanding your hormones to optimise your health and performance” I discuss how our lifestyle choices and behaviours around sleep, exercise and nutrition influence hormone networks and consequently our health.

Sleep for hormone health
Why is sleep such an essential component for health? Although being asleep is a physical state of inactivity, it is when many hormone networks are at their most active. For example, one of the main stimuli for growth hormone (GH) release is sleep. Despite its name, GH is not just about growth in children. All adults continue to produce GH and this is an important anabolic (tissue building) hormone. GH maintains a healthy body composition: favouring muscle over fat deposition. GH also plays a role in bone health.
Sleep for fitness
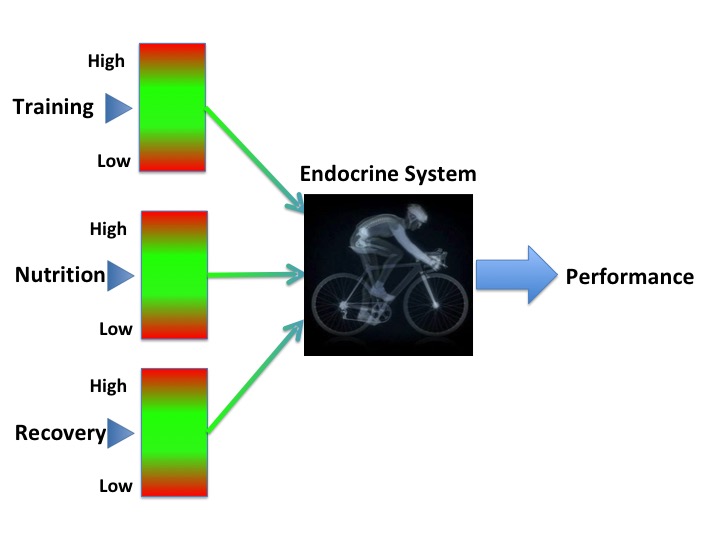
Another stimulus for GH release is exercise. However, you don’t get fitter in real time while you exercise. You get fitter when you are asleep. After stopping exercise and during sleep these two combined stimuli for GH release drive the positive adaptations to exercise. Sleep enables you to become citius, altius, fortius.
Sleep for sex steroid hormone networks
Sleep is also essential for other hormone networks, such as those of the reproductive axis, in both men and women. Studies show that men who have reduced sleep tend to have lower levels of testosterone and poorer bone health. Essentially if you do not have sufficient quality and quantity of sleep this has a negative effect on many aspects of both physical and mental health.
Sleep for metabolic health
Hormones that control appetite and satiety are linked with the sleep/wake cycle. People who have disrupted sleep patterns are more likely to struggle with blood glucose and weight control.
Timing of sleep
The timing of sleep is also important. Hormone networks run on a variety of internal biological clocks, known as biochronometers. The trick is to try and synchronise the timing of your behaviours with these internal biochronometers. If you have an “scheduling conflict” between external and internal clocks, this leads to a situation of circadian misalignment. Circadian misalignment can lead to many adverse consequences on mental and physical health, including metabolic and cardiovascular health. This negative combination can lead to metabolic syndrome which increases the risk of type 2 diabetes mellitus, cardiovascular disease and high blood pressure.
Consequences of disrupted sleep patterns
Shift workers, for example junior doctors, are at risk of developing circadian misalignment. Disrupted sleep patterns, clashing with internal hormone timing becomes a vicious circle. Poor sleep interferes with the diurnal variation of cortisol, which peaks as an awakening response. Disruption of this cortisol awakening response can disrupt subsequent night sleeping.
A degree of circadian entrainment is possible. In other words, our hormone clocks can adapt to slight changes in sleeping patterns. For example, getting up early for exercise training. It is also possible to reset internal biological clocks, as we do after a long-haul flight. This is because in our brain we have a biological light sensor which has direct communication with the manager of the hormone orchestra, conveniently situated in very close proximity in the brain. The timing of daily hormone release can be reset to correspond with local night and day timing. This contrasts to the situation of doing shift work, where you are continuously in conflict with night/day timing and internal hormone clocks.
Top tips for sleep to optimise hormone health
So, if there is one behaviour that you are going to improve this year, it should be sleep.
Sleep hygiene is the term used to cover strategies to ensure a good night’s sleep. One of the tops tips is to try and go to bed at a regular time, before midnight. A recent study shows that is these hours before midnight that are particularly valuable for hormone health. In fact, it is useful to set an alarm for going to bed.
Another strategy to help sleep is finding a bedtime “wind down” routine that suits you. For example, reading or listening to music. Looking at mobile electronic devices is not one of these. The reason being that the light emitted from these devices prevents the production of the sleep hormone melatonin.
When it comes to hormone health, sleep is indeed the chief nourisher. Sleep and other lifestyle choices to harness hormones for optimal health, through life, are explored in detail in “Hormones, Health and Human Potential: A guide to understanding your hormones to optimise your health and performance”.