Medically young, older athletes
Spot the differences?
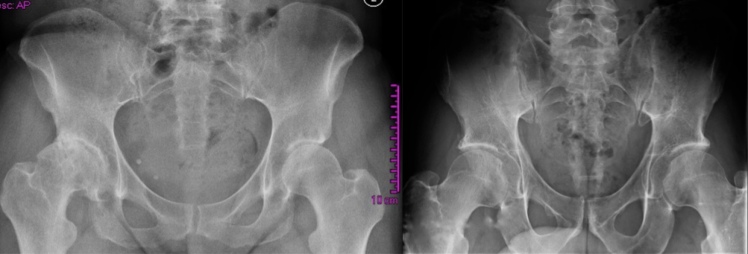
You don’t have to be a Radiologist to see that there are some differences between the two X-rays above. Both are from adults of the same age 51 years. Female on left as you look at screen and male on right. In both cases, these adults would be described as “medically young”. Always physically active and reasonably accomplished as athletes in their respective sport disciplines. Never smoked, never overweight, good nutrition.
As discussed at the recent conference at the Royal Society of Medicine (RSM) on “Sports Injuries and Sports Orthopaedics” in the session on the “Ageing Athlete”, there are challenges for athletes in Masters’ age groups, including mechanical joint issues associated with increasing age.
Looking at the male X-ray on right there is small gap between femoral head (ball-like structure) and acetabulum (socket in which femoral head lies). This gap is where the articular cartilage reduces friction between articulating surfaces of this ball and socket joint. In contrast in female X-ray on left of screen, this gap is reduced as cartilage has been worn away so that on right hip (left as you look at screen) bone is grinding on bone. Ouch!
Look again at the femoral heads (ball like structures). In the male these have smooth contours and are symmetrical on both sides. In contrast, in the female there is marked asymmetry with squashed appearance on right side (left of screen) of the femoral head with honeycomb appearance suggesting that there is cyst formation and impaction into socket of joint. This results in shorter leg and weakness of the bone architecture so more likely to compress further. Strangely the blood supply to femoral head is retrograde, meaning it flows backwards from origin of supplying blood vessel to provide vital nutrients to bone, which is a living tissue. If this blood supply is disrupted then the bone dies (avascular necrosis) and become more fragile. The femoral neck (slim area below femoral head) where blood supply courses, has been telescoped down and looks stubby compared to opposite side in female.
Although in the female, the right hip aches and is stiff, it is actually the left hip (right as you look at screen) that hurts more, both at rest and when trying to exercise. Why? If you look carefully on the upper boarder of acetabulum (socket) you will see small cysts. I imagine that pain is caused when the synovial fluid (lubricating fluid) in joint is forced into exposed bone, in hydraulic action especially when moving the hip joint.
So what to do? Total hip replacement (THR) is the only feasible option for the female above, due to extensive damage to the hip joints. Why are some people more prone to this type of joint damage? Apart from underlying medical pathologies that damage joints, the nature of some types of exercise can contribute. For example Ballet is demanding on the hip joint in terms of range of movement and load bearing. The individual can also be predisposed in biomechanical terms to joint issues: in the female X-ray above the femoral head is more exposed than the male.
Although the perception is that THR is more for the elderly wishing to be able to walk to the shops, with improvements in materials and technology used in hip protheses, there are examples of young athletes successfully returning to previous pre-operative levels of exercise training without pain. Recently a 28 year old male soloist dancer of the Paris Opera Ballet had a THR and returned to professional dancing. The medically young athlete will probably have the required motivation and physical ability to rehab effectively. A house in the south of France with private pool and climate for rehab outside would certainly add to motivation. Nevertheless, return to dancing at a professional level in a top level Ballet company after THR is remarkable as classical dance requires a unique combination of outstanding strength, control, proprioception and flexibility. At the conference at the RSM, during the lecture on “Can I run after my hip replacement?” hip replacements in the medically young, active population were reported to have good success rate with athletes able to return to previous level of sport with predicted lifespan of replacement of up to 25 years. Of course every individual athlete should weigh up the pros and cons. Taking up a new impact sport would probably not be sensible. Delaying surgery too long, apart from increasing pain, can compromise biomechanics and therefore replacement outcome. On the other hand, any operation carries a risk, however small and THR requires extensive rehabilitation in order to return to sport.
Deciding on the timing of THR in medically young, older athlete is not straight forward, especially if considering your own hips. Ultimately in such a person, the decision to go for surgery is based on quality of life and limitation to current sport activity, combined with the desire to return to previous level of activity, without the pain. What would you do?
For further discussion on Endocrine and Metabolic aspects of SEM come to the BASEM annual conference 22/3/18: Health, Hormones and Human Performance
References
Successful Ageing Dr N. Keay, British Association of Sport and Exercise Medicine 2017
Conference: Sports Injuries and Sports Orthopaedics, Royal Society of Medicine, 18/1/17, Session “The Ageing athlete”. Including lectures on: “Can I run after my hip replacement? Current recommendations for impact exercise following joint replacement” Mr Konan and “Managing acute injuries in worn joints” Mr Oussedik